
The Clinical Reality of Early Hair Loss: The Mirror Moment
In the field of hair restoration, the initial realization of androgenetic alopecia (pattern baldness) often occurs during what is colloquially known as the mirror moment. This is the morning when the bathroom lighting perfectly highlights a receding temporal hairline or a diffuse thinning across the vertex, making the scalp visibly apparent. For men in their early twenties, this sudden awareness can trigger profound psychological distress and an immediate, urgent desire for surgical intervention.
Consider the clinical vignette of a hypothetical 23-year-old patient, Mark. Experiencing aggressive temporal recession, Mark began dedicating excessive time each morning to meticulously styling his hair to conceal the progressive thinning. Driven by the fear of premature aging and the psychological burden of hair loss, he was prepared to liquidate his savings for an immediate hair transplant. Mark's situation is highly prevalent. However, the desperation to permanently fix the issue immediately frequently clashes with the biological reality of androgenetic alopecia, which is a chronic, progressive condition. The core question for patients like Mark is whether there exists an optimal clinical window or goldilocks zone for surgical hair restoration.
The Agitation: The Inherent Risks of Premature Surgical Intervention
Understanding the pathophysiology of hair loss is crucial before considering surgery. When a hair transplant is performed on a very young patient whose hair loss has not yet stabilized, several severe long-term complications can arise. The most prominent of these is the island effect. If a surgeon reconstructs a dense, juvenile hairline at age 22, the genetically susceptible native hair behind the transplanted follicles will likely continue to miniaturize and eventually shed. This progressive loss leaves the patient with a conspicuous, isolated tuft of transplanted hair at the anterior hairline, surrounded by a barren scalp, resulting in a highly unnatural aesthetic that requires immediate, and often complex, corrective surgery.
Furthermore, it is imperative to understand that donor hair—typically harvested from the safe donor area (SDA) at the occipital and parietal regions of the scalp—is a strictly finite resource. A patient only possesses a limited number of follicular units available for extraction without causing visible depletion in the donor zone. If a significant portion of this finite reservoir is exhausted at age 25 to reconstruct a hairline, there will be insufficient follicular units remaining to address the inevitable, and often more extensive, balding at the mid-scalp and vertex (crown) when the patient reaches age 45 or 50.
This biological limitation leads to a profound psychological and financial toll. Young patients who rush into surgery frequently find themselves trapped in a cycle of chase-up surgeries. They are continually forced to undergo subsequent procedures to bridge the expanding gap between the initial transplant and their receding native hair, leading to donor depletion, increased financial strain, and sustained anxiety.
The Solution: Understanding the Ideal Age Window for Restoration
Given the progressive nature of androgenetic alopecia, the general consensus among board-certified hair restoration surgeons is to defer surgical intervention until the patient is between the ages of 25 and 30, or ideally older. This recommendation is not arbitrary; it is rooted in biological maturity and the predictability of hair loss patterns. By the time a male patient reaches his late twenties to early thirties, his progression along the Norwood-Hamilton Scale becomes significantly more predictable.
Operating on a stable and predictable canvas allows the surgeon to formulate a comprehensive, lifelong master plan. The fundamental goal is to shift the paradigm from reactive surgery—frantically addressing the most recent areas of thinning—to strategic restoration, which accounts for the patient's future age, potential future loss, and the judicious management of the finite donor supply over a lifespan.
Six Evidence-Based Strategies for Navigating the Age Gap
For young men experiencing early-onset thinning, the period of waiting for surgical candidacy is not passive. There are highly effective, proactive protocols to manage the condition.
1. Stabilize Before You Operate
The foremost prerequisite for any young prospective patient is the stabilization of native hair. This is achieved through the disciplined use of FDA-approved medical therapies, primarily Finasteride (a 5-alpha-reductase inhibitor that reduces systemic DHT levels) and topical or oral Minoxidil (which prolongs the anagen growth phase). Committing to medical therapy for a minimum of 6 to 12 months can halt progressive shedding and, in many cases, induce the thickening of miniaturized hairs. If medical therapy successfully stabilizes the condition, a patient may find their surgical requirements reduced by hundreds or even thousands of grafts.
2. Map Your Family History (The Genetic Crystal Ball)
Androgenetic alopecia is a highly polygenic condition. Analyzing the hair loss patterns of older male relatives on both the maternal and paternal sides provides invaluable diagnostic insight. If a patient's father or maternal uncle exhibits a Norwood 6 or 7 pattern at age 50, the surgeon must assume the patient possesses a similar genetic trajectory. This necessitates a highly conservative surgical approach, designing a high and tight hairline to preserve the maximum number of grafts for future, extensive mid-scalp and crown restoration.
3. Prioritize Age-Appropriate Hairline Design
A successful hair transplant must remain aesthetically appropriate throughout the patient's entire life. The clinical objective is to design a hairline that looks natural and refined at age 30, and remains equally dignified at age 60. This requires opting for a slightly recessed, mature adult hairline, incorporating subtle temporal recessions. Designing a flat, juvenile hairline is fundamentally incompatible with the natural aging process of the human face and skull.
4. Obtain a Microscopic Evaluation of Donor Density
Age is merely one variable; the quantitative metrics of the donor zone are equally critical. Patients should seek a clinical consultation utilizing digital trichoscopy. This diagnostic tool provides precise measurements of follicular units per square centimeter, average hair shaft caliber, and the ratio of miniaturized to terminal hairs in the safe donor area. A patient with exceptionally high donor density and thick hair caliber might be cautiously considered for early intervention at age 26, whereas a patient with inherently low donor density must definitively wait until full stabilization is achieved.
5. Focus on Density Over Coverage
When younger patients do present as appropriate candidates, the surgical strategy should emphasize bolstering density within the existing forelock rather than aggressively lowering the anterior boundary. For instance, strategically utilizing 1,000 to 1,500 follicular unit grafts to thicken a diffuse frontal zone yields a significantly higher cosmetic impact with lower long-term risk than utilizing 3,000 grafts to aggressively reconstruct a low forehead.
6. Track Progression with Standardized Medical Photography
Self-assessment in a bathroom mirror is inherently subjective and prone to bias. The clinical standard is standardized medical photography. Patients should document their scalp every three to six months using consistent lighting, angles, and hair length. If these longitudinal records demonstrate no perceptible macroscopic progression over a 24-month period, the hair loss has likely stabilized. This verifiable stability makes the patient a significantly safer surgical candidate, providing an objective metric that supersedes chronological age.
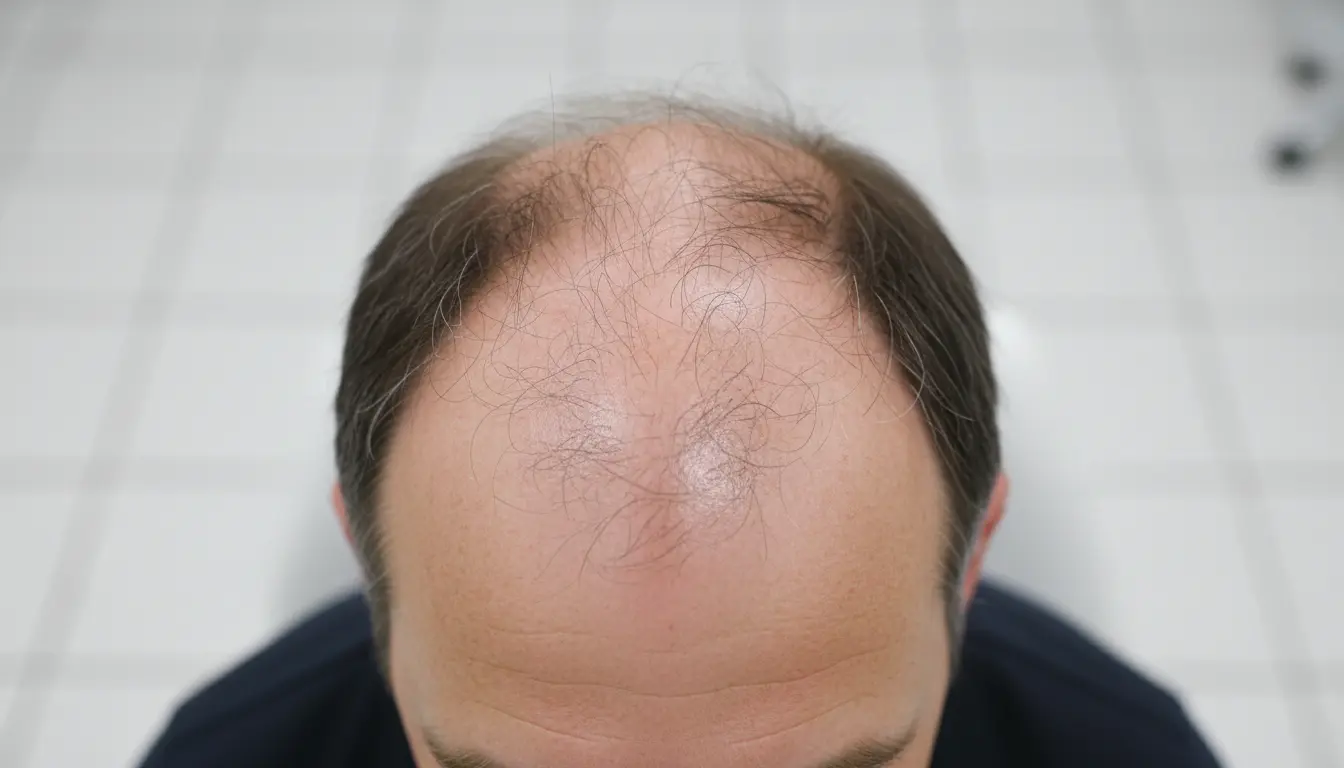
The Primary Clinical Error: The Low Hairline Trap
The most frequent error observed in consultations with young men is the insistence on recreating a juvenile hairline—the perfectly straight, dense anterior boundary typical of an adolescent. As the facial structure ages, the skin loses elasticity, and the native hair invariably recedes further back. A dense, low, transplanted wall of hair will inevitably begin to look like an artificial hairpiece. Furthermore, constructing this low hairline requires an exorbitant volume of grafts, severely depleting the donor reserve and leaving the patient entirely vulnerable when extensive balding inevitably strikes the mid-scalp and vertex. Expert, ethical surgeons will always advocate for a conservative initial start, prioritizing long-term aesthetic harmony over short-term gratification.
Conclusion: A Lifelong Commitment to Restoration
Ultimately, while chronological age is a crucial diagnostic variable, biological stability is the definitive metric that governs hair transplant candidacy. Surgical hair restoration is accurately described as a marathon, not a sprint. Patients must resist the urge for immediate, reactive intervention and instead collaborate with a certified physician to develop a scientifically sound, long-term master plan. By dedicating their twenties to medical stabilization and strategic planning, men can ensure they maintain a natural, aesthetically pleasing head of hair well into their fifties and beyond. If you are experiencing early-onset hair loss, the most critical next step is to schedule a comprehensive, professional consultation to objectively assess your Norwood stage, evaluate your donor density, and establish a personalized, evidence-based treatment protocol.


