I. Introduction: The "Invisible" Part of the Procedure
When patients research hair restoration, the focus is almost exclusively on the aesthetic outcome: the density of the hairline, the number of grafts, and the reputation of the surgeon. However, there is a critical component of the surgery that is frequently overlooked until the morning of the procedure: pain management.
Consider the case of "David," a 38-year-old technology executive. David approached his hair transplant with the rigorous analytical mindset of his profession. He researched Follicular Unit Excision (FUE) tech, vetted clinics for their survival rates, and understood the post-op care regimen perfectly. Yet, upon sitting in the surgical chair, David experienced a physiological freeze response at the sight of the initial anesthesia needle. Despite his preparation, he had not accounted for the sensory reality of the procedure.
This phenomenon highlights the "Anesthesia Gap." While patients prepare for the cosmetic result, they often ignore the logistical reality of the eight-hour surgical duration. This leads to the "Fidget Factor" and "Needle Dread." Enduring upwards of 2,000 micro-punctures while fully conscious can transform a positive aesthetic investment into a traumatic test of endurance.
In modern hair restoration, the standard of care is shifting. We are moving away from purely local approaches toward a "Hybrid Protocol." This method utilizes sedation not as a way to render the patient unconscious for the duration, but as a 15-minute "bridge" to ensure a pain-free entry into the local anesthesia phase.

II. Defining the Terms: What Are Your Options?
To make an informed decision regarding your surgical plan, it is essential to understand the medical distinctions between the available anesthetic modalities.
Local Anesthesia (The Foundation)
Local anesthesia is the non-negotiable foundation of hair transplant surgery. Regardless of sedation levels, every patient requires this. Surgeons typically employ a combination of Lidocaine (for immediate onset) and Bupivacaine (for long-duration numbing). These are administered via "ring blocks" around the circumference of the scalp, effectively severing the pain signals from the scalp nerves to the brain. Once established, the scalp becomes a sensation-free zone.
The 15-Minute Sedation (The "Bridge")
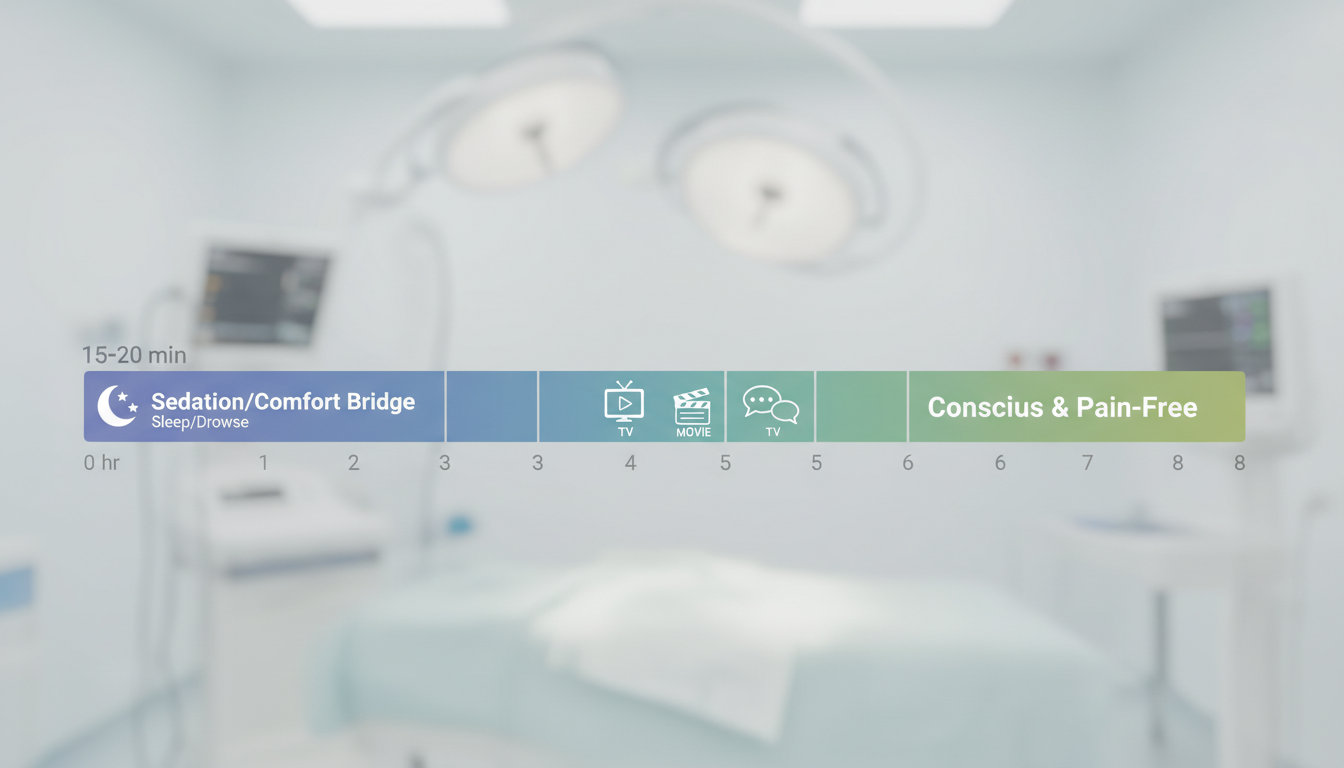
Modern clinics increasingly utilize intravenous (IV) or potent oral sedation specifically for the initial administration of the local anesthesia. This is the "bridge." The objective is to sedate the patient deeply enough that they do not feel the initial injections of the ring block. This phase typically lasts 15 to 20 minutes. Once the scalp is fully numbed, the sedation is tapered off, allowing the patient to return to full consciousness while remaining pain-free.
General Anesthesia
General anesthesia involves complete unconsciousness and requires intubation to support breathing. In the context of hair restoration, general anesthesia is widely considered contraindicated due to the unnecessary risk profile. The physiological risks of deep unconsciousness outweigh the benefits for a cutaneous procedure where local anesthesia is highly effective.
III. The Core: 5 Things Every Candidate Needs to Know
Understanding the interplay between patient physiology and anesthesia is vital for setting realistic expectations. Here are the five critical factors regarding the Hybrid Protocol.
1. The "15-Minute Bridge" vs. The Marathon
A common misconception is that sedation is an all-or-nothing choice. Patients fear losing an entire day to grogginess. However, from a clinical perspective, the only painful portion of a hair transplant is the administration of the local anesthetic injections.
Under the Hybrid Protocol, sedation acts as a "fast-forward" button. You are sedated specifically for the discomfort of the needles. Once the local anesthesia has achieved efficacy (usually within 15 minutes), the patient is awakened. You are then wide awake, able to converse, watch movies, or use your phone, but the surgical site is 100% numb. The "marathon" of the surgery is conducted comfortably, without the need for continuous systemic sedation.
2. The "Fidget Factor" & Surgical Precision
Patient anxiety has a direct correlation with surgical outcomes. When a patient is anxious or in pain during the initial numbing phase, they exhibit micro-movements—tensing the neck, shifting the shoulders, or twitching. In microsurgery, where grafts are extracted at a sub-millimeter level, stability is paramount.
By utilizing the sedation bridge, the patient remains perfectly still during the critical setup phase. This allows the surgeon to administer the local blocks with greater accuracy and speed, ensuring a more thorough numbing effect and reducing the total time the patient spends in the chair.
3. Safety: BMI, Sleep Apnea, and Monitoring
While the Hybrid Protocol is generally safe, it introduces medical considerations that local-only procedures do not. This is particularly relevant for the 40+ demographic. Clinics adhering to high safety standards will require a review of Body Mass Index (BMI) and a history of Obstructive Sleep Apnea (OSA). Sedation can relax the airway muscles; in patients with undiagnosed sleep apnea, this can lead to oxygen desaturation. Therefore, even a 15-minute sedation requires continuous monitoring of vitals, including pulse oximetry and blood pressure, to ensure hemodynamic stability.
4. The "Post-Op Pivot"
The choice of anesthesia dictates the immediate postoperative logistics.
Local-Only: Since there is no systemic impairment, patients can theoretically drive themselves home, though it is rarely recommended due to fatigue.
Sedation: Even with a short-duration "bridge," the metabolites of sedatives remain in the bloodstream. Patients are clinically clear-headed within an hour, but their reaction times may be delayed. Consequently, discharge protocols strictly require a designated driver or medical transport. This logistical requirement must be planned in advance.
5. Cost-Benefit Analysis: The "Comfort Premium"
Implementing IV sedation or monitored anesthesia care (MAC) requires additional resources: an anesthesiologist or CRNA, monitoring equipment, and recovery protocols. This typically adds a "comfort premium" of $500 to $1,500 to the total procedure cost.
From a patient experience standpoint, this is often viewed as a high-value expenditure. For those with needle phobia, this cost effectively neutralizes the primary barrier to surgery. The reduction in psychological trauma and the increase in physical comfort usually justify the expense.

IV. Actionable Tips for a Pain-Free Experience
Regardless of whether you choose the Hybrid Protocol or stick to local anesthesia, there are clinical strategies to mitigate discomfort.
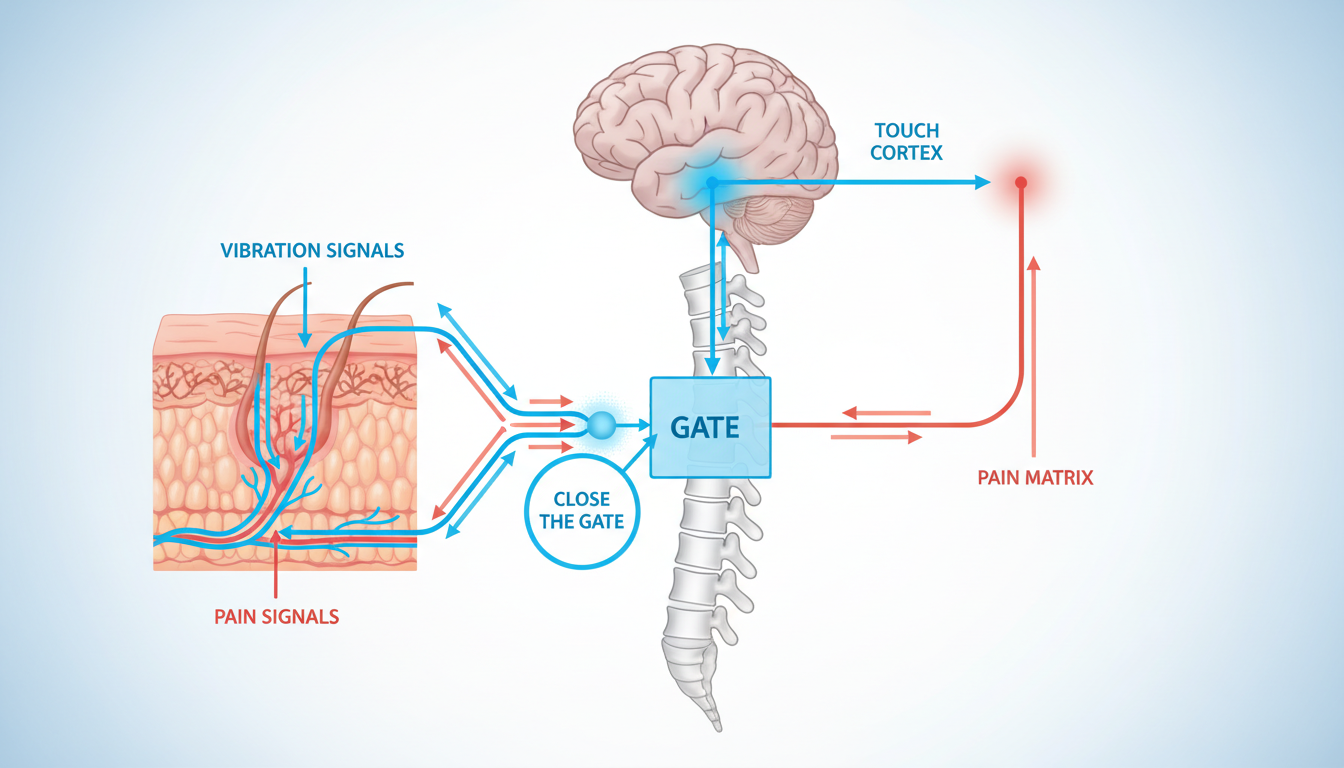
Tip 1: The "Vibration Tool" (Gate Control Theory)
Ask if your surgeon uses a vibration device during injections. The "Gate Control Theory" of pain posits that non-painful input (vibration) closes the nerve "gates" to painful input (injections), significantly reducing the sensation of the needle.
Tip 2: Request "Buffered" Anesthesia
Lidocaine is naturally acidic, which causes the characteristic "burn" upon injection. Adding sodium bicarbonate to the solution buffers the pH to neutral levels, eliminating the sting and leaving only the pressure of the injection.
Tip 3: The "Pre-Med" Strategy
If IV sedation is unavailable or outside your budget, discuss an oral anxiolytic (such as diazepam) taken 30 to 45 minutes prior to the procedure. While less potent than IV, it dampens the nervous system response.
Tip 4: Hydration & Caffeine Control
Refrain from caffeine on the morning of surgery. Caffeine is a stimulant that can heighten anxiety and counteract the calming effects of sedatives. Furthermore, it acts as a diuretic, potentially complicating the long surgical session.
Tip 5: Establish the "Zinger" Signal
During the extraction phase, you may occasionally feel a sharp sensation if the anesthesia wears off in a specific spot. Establish a non-verbal hand signal with your surgeon beforehand. This allows you to request a "top-up" of anesthesia without moving your head or speaking, maintaining the sterile field.
Tip 6: Noise-Canceling Strategy
For some patients, the sound of the FUE punch tool creates sensory discomfort. High-quality noise-canceling headphones are highly recommended to dissociate from the clinical environment.
V. The Common Mistake: "The Hero Complex"
A frequent error observed in male patients is the "Hero Complex"—choosing local-only anesthesia to "tough it out," despite harboring significant anxiety or needle phobia.
From a medical standpoint, this is counterproductive. High levels of anxiety trigger the release of cortisol and adrenaline. These stress hormones induce vasoconstriction (narrowing of blood vessels) and elevate blood pressure. This physiological state can make the scalp tissue tighter and more difficult to work with, and paradoxically, can increase bleeding once the extraction begins. A relaxed patient is physically easier to operate on, often resulting in better graft integrity.
VI. Conclusion: Empowerment Through Knowledge
The narrative surrounding hair transplantation is changing. It is no longer just about the result; it is about the experience. The Hybrid Protocol represents the gold standard for the modern patient, offering a sophisticated balance between safety, comfort, and surgical efficacy.
By understanding the role of the "15-minute bridge," you can eliminate the fear of pain from your decision-making process. You are investing in your appearance and your confidence; do not let a temporary hurdle prevent you from achieving a lifetime of results. Discuss your anesthesia options with your surgeon during the consultation to ensure a plan that aligns with both your medical history and your comfort levels.


